|
|
Developmental Biology - Immune System
Flipping A Switch Against Lupus
The PD-1H molecule is critical to immunity against attacks that are hallmarks of Lupus and several other cancers...
Autoimmunity can result when the intricate checks and balances of the immune system are disrupted. In the last decade, scientists have discovered that blocking a key immune system regulator helped unleash the body's natural defenses against several forms of cancer, opening up a new era of cancer immunotherapy.
Now Yale scientists have essentially flipped this script and found that when impaired, a molecularly similar regulator can cause damaging immune system attacks on skin and organs that are the hallmark of the autoimmune disease Lupus, as reported Dec. 11, 2019 in the journal Science Translational Medicine.
Their study results help explain the origins of Lupus, suggesting novel ways researchers might be able to restore function to this inhibitor. If so, they can provide much needed new therapy to treat the disease.
The immune system has a series of regulators designed to prevent it from attacking tissues in its host's body in autoimmune diseases. Yale researchers found that mice lacking an immune system inhibitor called programmed death-1 homolog, or PD-1H, spontaneously developed symptoms resembling two forms of lupus (1) systemic, in which the immune system attacks multiple organs; and (2) cutaneous, which is marked by pronounced skin deformities.
"This molecule is clearly involved in inhibiting lupus, but it seems to be selective as it does not have the same effect in several other autoimmune diseases."
Lieping Chen PhD, the United Technologies Corporation Professor in Cancer Research, and Professor of Immunobiology, Dermatology & Medicine at Yale University, New Haven, Connecticut, USA. and senior author.
PD-1H is molecularly similar to the more commonly known PD-1 molecule, which also helps suppress immune system responses. Chen was a pioneer in identifying and developing inhibitors to PD-1 which frees T cells to attack several forms of cancer. Several labs have also tried to use PD-1H as a cancer treatment but so far have been unsuccessful.
Chen believes his findings suggest that with lupus, the function of PD-1H is critical. When it is impaired, patients are vulnerable to immune system attacks on their skin and multiple organs which are hallmarks of the disease.
Lupus patients currently have very limited options for treatment, but these new findings suggest a novel approach called protein fusion might mimic PD-1H and help control the immune system and combat the disease. Xue Han and Matthew Vesely are co-lead authors of the study.
Supporting A Suppressor for Lupus Treatment
Han et al. discovered a potential treatment target for lupus erythematosus: the inhibitory receptor PD-1H. PD-1H knockout mice on a BALB/c background developed cutaneous lesions and were more susceptible to pristane-induced autoimmunity. Treating lupus-prone MRL/lpr mice with an antibody that activated PD-1H reduced skin symptoms and some markers of autoimmunity. The antibody was shown to act on myeloid cells and T cells and could potentially restore immune balance in patients with lupus.
Abstract
Systemic lupus erythematosus (SLE) and discoid lupus erythematosus (DLE) of the skin are autoimmune diseases characterized by inappropriate immune responses against self-proteins; the key elements that determine disease pathogenesis and progression are largely unknown. Here, we show that mice lacking immune inhibitory receptor VISTA or programmed death-1 homolog (PD-1H KO) on a BALB/c background spontaneously develop cutaneous and systemic autoimmune diseases resembling human lupus. Cutaneous lupus lesions of PD-1H KO mice have clustering of plasmacytoid dendritic cells (pDCs) similar to human DLE. Using mass cytometry, we identified proinflammatory neutrophils as critical early immune infiltrating cells within cutaneous lupus lesions of PD-1H KO mice. We also found that PD-1H is highly expressed on immune cells in human SLE, DLE lesions, and cutaneous lesions of MRL/lpr mice. A PD-1H agonistic monoclonal antibody in MRL/lpr mice reduces cutaneous disease, autoantibodies, inflammatory cytokines, chemokines, and immune cell expansion. Furthermore, PD-1H on both T cells and myeloid cells including neutrophils and pDCs could transmit inhibitory signals, resulting in reduced activation and function, establishing PD-1H as an inhibitory receptor on T cells and myeloid cells. On the basis of these findings, we propose that PD-1H is a critical element in the pathogenesis and progression of lupus, and PD-1H activation could be effective for treatment of systemic and cutaneous lupus.
Authors
Xue Han, Matthew D. Vesely, Wendy Yang, Miguel F. Sanmamed, Ti Badri, Jude Alawa, Francesc López-Giráldez, Patricia Gaule, Sang Won Lee, Jian-Ping Zhang, Xinxin Nie, Ala Nassar, Agedi Boto, Dallas B. Flies, Linghua Zheng, Tae Kon Kim, Gilbert W. Moeckel, Jennifer M. McNiff and Lieping Chen.
Acknowledgments
The research was primarily funded by Boehringer Ingelheim, which had investigated PD-1H as a potential cancer treatment, and by a United Technologies endowment.
The research was supported by the National Institutes of Health (NIH F31EY028022-03, RO1EY019498, RO1EY013528, P30EY003176).
This research was funded through the Biosphere Evolution, Transitions and Resilience (BETR) programme, which is co-funded by the Natural Environment Research Council (NERC) and Natural Science Foundation of China (NSFC).
Declaration of Interests
The authors declare no competing interest.
Return to top of page.
| |
|
Dec 17 2019 Fetal Timeline Maternal Timeline News
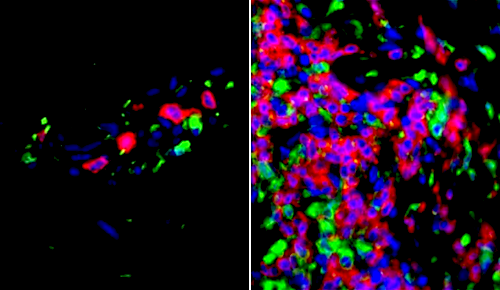 Skin samples from lupus patients show heightened activity in immune system genes. CREDIT Chen Laboratory.
|



