|
|
Developmental Biology - Male Puberty
How Male Puberty Affects Normal Growth and Cancer
In the first genome analysis of human male puberty, science sees how testosterone impacts stem cells...
The Huntsman Cancer Institute (HCI), University of Utah (U of U) has now outlined distinct and critical changes to male stem cells during adolescence. Researchers were also able to record how testosterone, and cells that produce testosterone, impact stem cells in male reproductive organs. The research is published in Cell Stem Cell.
The study was led by Bradley Cairns PhD, Professor and Chair of Oncological Sciences at U of U. Cairns is also a cancer researcher at HCI, working in collaboration with Jingtao Guo PhD, a postdoctoral fellow and with James Hotaling MD, Associate Professor of surgery at U of U, and Anne Goriely PhD, Associate Professor of Human Genetics at the University of Oxford, United Kingdom.
Puberty spurs numerous developmental changes in humans as well as in other mammals. Hallmarks include physical characteristics easily visible to the naked eye, like rapid growth, and hormonal changes which signal maturation in the body preparing it for reproduction.
Today, new genomic technologies can examine the expression of thousands of genes within one individual cell of an entire organ.This provides unprecedented insight into cellular behavior during puberty in the testis which make and store sperm and produce testosterone.
There are at least 3 cell types in the testis:
Spermatogonial Stem cells which generate sperm production
Niche cells which help form parts of the testis such as:
Seminiferous Tubules within which sperm forms
This study characterized how just prior to puberty, numbers of spermatogonial stem cells expands significantly. Just as the human body changes from infancy to adulthood, sex cells also undergo major changes with maturity.
As stem cells progress toward meiosis, cell division that splits the number of chromosomes from the parent cell in half, also separates male X and Y sex chromosomes to create cells that will ultimately result in either male (Y-containing) or female (X-containing) children.
Late in puberty, these stem cells create mature sperm, which includes a tail piece for motility. The research showed two of the cells that form the stem cell niche to chaperone this process - myoid cells and Leydig cells - come from a common cell which matures in early puberty.
A major new insight of this study comes from the first genomic analysis of testis of adult transfemales (assigned to be male at birth, but who later self-identify as female).
For transfemales, gender confirmation surgery is preceded by hormone therapy to suppress testosterone. This enables examination of testis without testosterone. Examining testies donated following surgery, researchers got critical insights into how testosterone maintains testis development, showing that stem cells (and other cells) revert to earlier states of development when compared to samples taken from adolescent males.
The research identified that testosterone is critical to maintaining a mature state in testis. If testosterone is no longer present, testis revert to an earlier developmental state. When sexual development goes awry in puberty, challenges can result infertility being a relatively common issue.
The study also informs an understanding of cancer and other diseases arising from errors in cellular processes. Cairns: "The majority of the time, testicular cancers arise when stem cells in the testis are misregulated. We want to understand how these changes can cause testicular tumors; however, we need to know what should normally happen before we can identify ways to prevent or more effectively treat these cancers."
In juveniles, cancers and reproductive health intersect in a medical process called oncofertility the study of "fertility retention" in adolescent and young adult cancer patients. Reproductive health and fertility can be impacted by cancer, or as a side effect of cancer treatment.
"Some chemotherapies can result in young men with cancer not being able to have children as chemotherapy changes stem cells.
My hope and expectation is that our research will provide options to support reproductive health in these young men through understanding how stem cells survive, are supported and develop."
Bradley Cairns PhD, Professor and Chair, Oncological Sciences, U of U.
Highlights
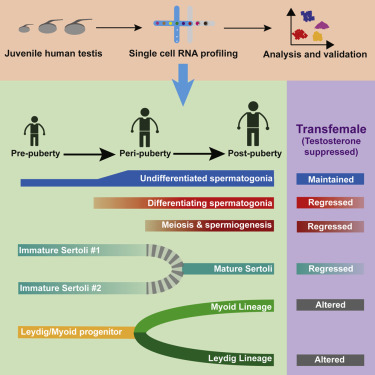
A transcriptional single-cell atlas of the developing testes during human puberty
Distinctive phases of germ cell differentiation occur during puberty
Identification of a common progenitor for Leydig and myoid cells prior to puberty
Partial reversal of Sertoli and germ cell maturation upon testosterone suppression
Summary
The human testis undergoes dramatic developmental and structural changes during puberty, including proliferation and maturation of somatic niche cells, and the onset of spermatogenesis. To characterize this understudied process, we profiled and analyzed single-cell transcriptomes of ~10,000 testicular cells from four boys spanning puberty and compared them to those of infants and adults. During puberty, undifferentiated spermatogonia sequentially expand and differentiate prior to the initiation of gametogenesis. Notably, we identify a common pre-pubertal progenitor for Leydig and myoid cells and delineate candidate factors controlling pubertal differentiation. Furthermore, pre-pubertal Sertoli cells exhibit two distinct transcriptional states differing in metabolic profiles before converging to an alternative single mature population during puberty. Roles for testosterone in Sertoli cell maturation, antimicrobial peptide secretion, and spermatogonial differentiation are further highlighted through single-cell analysis of testosterone-suppressed transfemale testes. Taken together, our transcriptional atlas of the developing human testis provides multiple insights into developmental changes and key factors accompanying male puberty.
Authors
Jingtao Guo, Xichen Nie, Maria Giebler, Hana Mlcochova, Yueqi Wang, Edward J. Grow, Robin Kim, Melissa Tharmalingam, Gabriele Matilionyte, Cecilia Lindskog, Douglas T. Carrell, Rod T. Mitchell, Anne Goriely, James M. Hotaling, Bradley R. Cairns
Acknowledgments
This research was supported by the National Cancer Institute grants P30 CA042014, the Howard Hughes Medical Institute, and Huntsman Cancer Foundation.
About Huntsman Cancer Institute:
Huntsman Cancer Institute (HCI) at the University of Utah is the official cancer center of Utah. The cancer campus includes a state-of-the-art cancer specialty hospital as well as two buildings dedicated to cancer research. HCI treats patients with all forms of cancer and is recognized among the best performing cancer hospitals in the country by U.S. News and World Report. As the only National Cancer Institute (NCI)-Designated Comprehensive Cancer Center in the Mountain West, HCI serves the largest geographic region in the country, drawing patients from Utah, Nevada, Idaho, Wyoming, and Montana. More genes for inherited cancers have been discovered at HCI than at any other cancer center in the world, including genes responsible for hereditary breast, ovarian, colon, head, and neck cancers, along with melanoma. HCI manages the Utah Population Database, the largest genetic database in the world, with information on more than 11 million people linked to genealogies, health records, and vital statistics. HCI was founded by Jon M. and Karen Huntsman.
Return to top of page.
| |
|
Jan 13 2020 Fetal Timeline Maternal Timeline News
 Major changes occur in human puberty that affect reproductive health. Infertility is relatively common about 50 percent of the time affecting men. Knowing how cells develop helps us determine outcomes that might ignite infertility. CREDIT Pinterest.
|




