|
|||||||||||||||
|

CLICK ON weeks 0 - 40 and follow along every 2 weeks of fetal development
|
||||||||||||||||||||||||||||
|
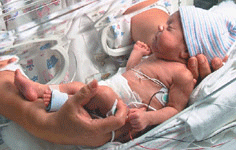
Mom's preeclampsia increases risk to baby's heart Pregnant women with preeclampsia have a higher risk of delivering an infant with a congenital heart defect. An extensive study of 1.9 million mother and infant pairs at the University of Montreal Hospital Research Centre (CRCHUM) has shown significant association between preeclampsia in mothers and their newborns from early pregnancy. Congenital heart defects are the most common anomalies in infants, affecting every 8 births in a 1,000. They are a major cause of infant illness and death, despite significant medical care advancements. The origin of heart defects is sometimes hereditary, but risk factors were mostly unknown. Researchers had considered a possible link with preeclampsia, a pregnancy disorder characterized by high blood pressure and excess protein in the urine (proteinuria).
Researchers decided to examine hospital records of live births for the entire province of Quebec - making up of a quarter of Canada's population - between 1989 and 2012. All women who delivered an infant after 20 weeks of pregnancy during this period were included — and 1,942,072 neonates. Overall, 17,296 neonates or 8.9 per 1,000, had heart defects. Prevalence was higher for infants of women with preeclampsia than without (16.7 vs. 8.6 per million). The most frequent heart defects were non-critical, such as septal defects, characterized by a hole in the wall separating the ventricles or atria of the heart and causing blood flow problems.
Preeclampsia is detectable around the 20th week of pregnancy and can progress to full eclampsia endangering the life of the mother and child. Currently, women diagnosed with preeclampsia are closely monitored to see if their baby is developing normally. Most infants with congenital heart defects can be saved. They are treated with medications, non-invasive procedures, or surgery.
Abstract Objective To determine the prevalence of congenital heart defects in offspring of women with preeclampsia. Design, Setting, and Participants Population-level analysis of live births before discharge, 1989-2012, was conducted for the entire province of Quebec, comprising a quarter of Canada’s population. All women who delivered an infant with or without heart defects in any Quebec hospital were included (N = 1?942?072 neonates). Exposures Preeclampsia or eclampsia with onset before or after 34 weeks of gestation. Main Outcomes and Measures Presence of any critical or noncritical congenital heart defect detected in infants at birth, comparing prevalence in those exposed and not exposed to preeclampsia. Results The absolute prevalence of congenital heart defects was higher for infants of women with preeclampsia (16.7 per 1000 [1219/72?782]) than without it (8.6 per 1000 [16?077/1?869?290]; prevalence ratio [PR], 1.57; 95% CI, 1.48 to 1.67). Infants of preeclamptic women had no increased prevalence of critical heart defects (123.7 vs 75.6 per 100?000 [90/72?782 vs 1414/1?869?290]; PR, 1.25; 95% CI, 1.00 to 1.57; prevalence difference [PD], 23.6 per 100?000; 95% CI, −1.0 to 48.2) but did have an increased prevalence of noncritical heart defects (1538.8 vs 789.2 per 100?000 [1120/72?782 vs 14?752/1?869?290]; PR, 1.56; 95% CI, 1.47 to 1.67; PD, 521.1 per 100?000; 95% CI, 431.1 to 611.0) compared with infants of nonpreeclamptic women. Among specific defects, prevalence was greatest for septal defects. When stratified by variant of preeclampsia, infants of women with early onset (<34 weeks) preeclampsia had greater prevalence of critical heart defects (364.4 per 100?000 [20/5488]; PR, 2.78; 95% CI, 1.71-4.50; PD, 249.6 per 100?000; 95% CI, 89.7-409.6) and noncritical heart defects (7306.9 per 100?000 [401/5488]; PR, 5.55; 95% CI, 4.98-6.19; PD, 6089.2 per 100?000; 95% CI, 5350.0-6828.3), whereas infants of women with late onset (≥34 weeks) did not. Conclusions and Relevance In this population-based study, preeclampsia was significantly associated with noncritical heart defects in offspring, and preeclampsia before 34 weeks was associated with critical heart defects. However, the absolute risk of congenital heart defects was low. The study "Association Between Preeclampsia and Congenital Heart Defects," was published online in JAMA, The Journal of the American Medical Association, on October 20. The study was supported by the Canadian Institutes of Health Research (CIHR) (MOP-130452). Dr. Auger was supported by a career award from the Fonds de recherche du Québec - Santé (FRQS) (Grant 25128). The authors state that the funding organizations were not involved in the design and conduct of the study or in the publication of the results. For more information: http://jama.jamanetwork.com/article.aspx?articleid=2463255 |
Oct 29, 2015 Fetal Timeline Maternal Timeline News News Archive
|
||||||||||||||||||||||||||||