|
|
Common gene links obesity to diabetes
The P53 tumor suppressor gene helps every bit of our general metabolism work. A new study reveals how it may have functioned in our early ancestors — and how when mutated, it turns into cancer.
Metabolism comes in two phases: anabolism, which produces chemical compounds needed for cells to function — and catabolism, the breakdown of molecules to make energy which also produces waste. What we eat, nutrition, is the key to metabolism. It provides fuel to be broken down into calories — the energy units essential in building, upkeep, and repair of tissues.
P53 is a tumor suppressor gene known as the "guardian of the genome" as it normally protects against cancer, unless mutated or made inactive when it is then found in the majority of cancers.
Now, researchers at The Wistar Institute make the case that p53 is also the "guardian of obesity." They found that a variant of P53 is heavily related to metabolism, the breakdown of foods to build and rebuild cells, but may also lead to obesity and type 2 diabetes.
Their study results are published in the journal Cell Reports.
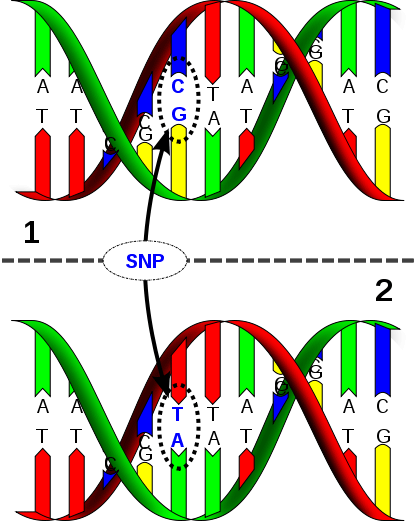
To understand why this crucial gene functions so differently across human populations, Maureen Murphy PhD, professor and program leader of the Molecular and Cellular Oncogenesis Program at Wistar, and her colleagues have focused on SNPs (single nucleotide polymorphisms).
SNPs are single gene variations at points along a DNA sequence.
In p53, the most common SNP occurs on the amino acid 72, coding for either of two amino acids: Proline (P72) or Arginine (R72).
For decades, the R72 variant (ARGININE) in p53 was found in people who lived farther away from the Equator — in colder climates — along with an increase in body mass and a susceptibility to type 2 diabetes. But, no one understood why.
Murphy and her colleagues examined mice with either the P72 (Proline) variant or the R72 (Arginine) variant to find the answer. Both types of mice were fed a normal diet for 10 weeks and then given a high-fat diet for eight weeks.
While on the normal diet, R72 (Arginine) variant mice showed a mild increase in weight gain, but a much more significant weight gain when switched to a high-fat diet — at least a 20 percent greater increase in body fat in R72 (Arginine) mice than in P72 (Proline) mice.
Glucose tolerance tests showed that following a high fat diet, R72 (Arginine) mice developed pre-diabetic symptoms and insulin resistance.
To confirm that a high-fat diet led to metabolic disorders in R72 (Arginine) mice, researchers fed the two groups a normal diet for 18 weeks instead of switching to a high-fat diet. No difference in glucose tolerance was observed between the two groups, confirming that the high-fat diet was responsible for the negative metabolic changes.
"Unlike the majority of other oncogenes and tumor suppressor genes, the p53 gene has variations that change it's processing of fat. For years, no one understood why such an important tumor suppressor would show genetic variation, much less in response to latitude.
"Now we think we understand why: the R72 (Arginine) variant may have arisen and been selected for in colder climates because it increases the body's ability to store fat. Unfortunately, this can also lead to increased risk for obesity, fatty liver disease and diabetes."
Maureen Murphy PhD, Professor and Program Leader, the Molecular and Cellular Oncogenesis Program at Wistar Institute, lead author of the study.
Murphy and her colleagues also identified two genes — Npc1l1 and Tnf — which are controlled by p53 and are noticeably different in the livers of R72 (Arginine) mice as compared with P72 (Proline) mice.
Npc1l1 has been linked to cholesterol absorption while Tnf is associated with obesity-induced insulin resistance.
Both genes act as "early-responders" in a high-fat diet, initiating the development of obesity and non-alcoholic fatty liver disease in the R72 (Arginine) mice. Since drugs that specifically inhibit these two genes already exist, the scientists fed them daily to R72 mice as treatment. Used together, both inhibitors led to significant decreases in weight gain and fat accumulation in R72 (Arginine) mice.
The study may also have provided an evolutionary explanation for differences in populations living farther from the Equator.
Our ancestors may have undergone a change in processing R72 (Arginine) to promote energy storage in cold climates and during times of famine. However, in our modern world this gene variant is unneeded and leads to increased risk for obesity and type 2 diabetes.
Obesity is also a risk factor for certain types of cancer, so Murphy's findings may also explain why people with the R72 (Arginine) variant on p53 might be predisposed to cancer.
"Not only does this study provide a more solid foundation for the link between p53 and metabolism, it also shows that targeting Npc111 and Tnf may be effective strategies for treating diabetes," adds Che-Pei Pat Kung PhD, a postdoctoral fellow in Maureen Murphy's laboratory, and first author of the study.
Wistar's Business Development team will be making the human p53 knock-in mouse models in this paper widely available to both academic and industry development partners interested in exploring the link between p53 and metabolism.
Abstract Introduction
The p53 tumor suppressor protein has a well-established role in the suppression of cancer (Levine and Oren, 2009). This protein confers its tumor-suppressive activities predominantly by acting as a transcription factor, transactivating over 200 different target genes. p53 has also been found to be a critical factor governing innate and adaptive immune responses, reproduction, development, neural degeneration, and aging (Chang et al., 2012, Danilova et al., 2008, Levine et al., 2011, Menendez et al., 2013, Poyurovsky and Prives, 2010). More recently, the relationship between p53 and metabolism has become the focus of new studies, particularly with the revelation that the role of p53 in metabolism may be essential to its tumor suppressor function (Li et al., 2012, Long et al., 2013, Maddocks et al., 2013, Vousden and Ryan, 2009). Additionally, considerable evidence points to a crucial role for p53 in metabolic diseases such as cardiovascular disease, obesity, and type 2 diabetes (Minamino et al., 2009, Ortega et al., 2014, Sano et al., 2007, Tavana et al., 2010).
This work was supported by the National Institutes of Health grants R01 CA102184, P01 CA114046-07, the Penn Diabetes Research Center Mouse Phenotyping Core grant P30DK19525, and the Penn Molecular Pathology and Imaging Core grant P30DK050306. Co-authors of this study from The Wistar Institute include Subhasree Basu and Qin Liu. Other co-authors include Sakina Khaku, Donna George, Julia I-Ju Leu, Frederick Anokye-Danso, and Rexford S. Ahima from the Perelman School at the University of Pennsylvania School of Medicine in Philadelphia.
The Wistar Institute is an international leader in biomedical research with special expertise in cancer research and vaccine development. Founded in 1892 as the first independent nonprofit biomedical research institute in the country, Wistar has held the prestigious Cancer Center designation from the National Cancer Institute since 1972. The Institute works actively to ensure that research advances move from the laboratory to the clinic as quickly as possible. wistar.org.
Return to top of page
|
|
|
Mar 8, 2016 Fetal Timeline Maternal Timeline News News Archive
|